HOW WE TREAT PHOBIA
Life-changing online care for phobia
Our providers understand the challenges of phobia, and have real-world experience helping people just like you.
Start with a free assessment
HOW WE TREAT PHOBIA
Our providers understand the challenges of phobia, and have real-world experience helping people just like you.
Start with a free assessment
Our Care
Different people experience phobia in different ways. That’s why our providers work 1:1 with you to personalize treatment to your unique needs.
When medication is necessary, our psychiatric providers analyze 100+ data points to determine the most tolerable and effective prescription for you.
Our program combines cognitive and behavioral therapy with independent skill practice—all of which have been clinically proven to work for a wide range of symptoms.
Mental Health condition
People with phobias often have panic attacks when faced with the thing they fear. The symptoms of the panic attack can occur suddenly and without warning.

Phobia is an intense, persistent, irrational fear of a specific situation, activity, object, or person. Usually, the feelings of fear are significantly greater than the actual danger or threat. People with phobias are highly distressed and preoccupied about feeling the fear, and often will go to great lengths to avoid the object or situation in question.
There are five different types of specific phobias. These include: Animal Type (e.g. dogs, snakes, spiders), Natural Environment Type (e.g., heights, storms, water), Blood-Injection-Injury Type (e.g. fear of seeing blood, receiving a blood test or shot), Situational Type (e.g., airplanes, elevators, driving, enclosed places), and Other Types (e.g., phobic avoidance of situations that may lead to choking, vomiting, or contracting an illness).

In addition to overwhelming feelings of anxiety, a panic attack can cause physical symptoms, such as:
In addition to the physical symptoms, psychological symptoms may also occur. These include:
HOW IT WORKS

Let your provider know how you’re feeling, get to know you, and provide 1:1 support.
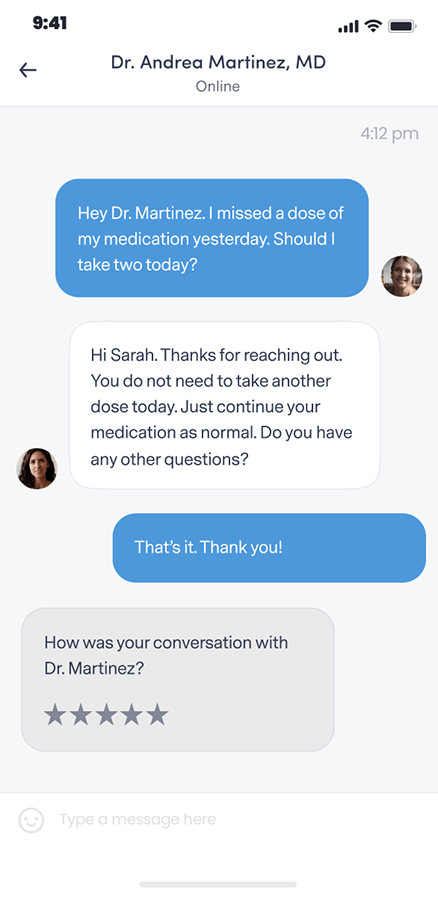
Get questions or concerns off your chest between video visits by messaging your provider at any time.
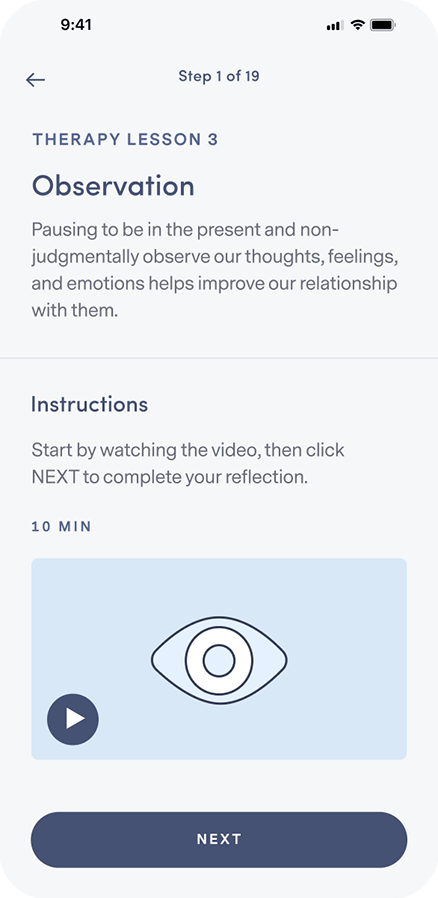
Learn how to integrate new thought and behavior patterns into your daily life.
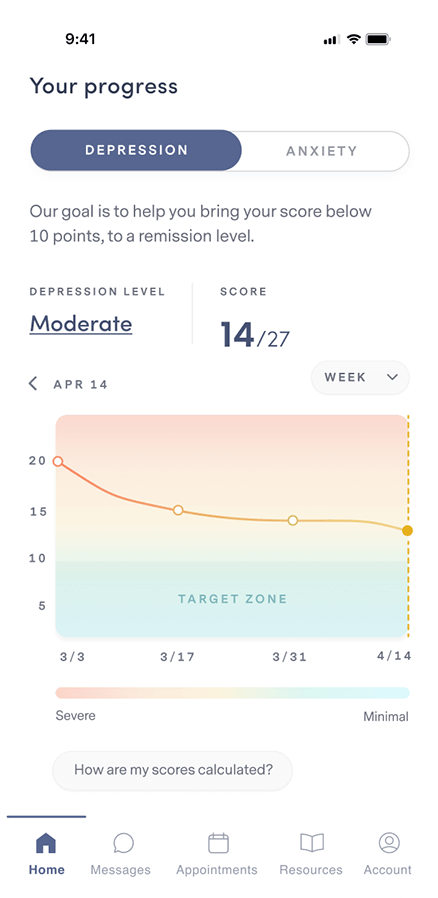
Complete weekly check-ins so your provider can track your progress and, if necessary, adjust your treatment and/or medication.
Our plan options
Because quality mental health care shouldn’t be out of reach for anyone.
PERSONALIZED
clinically-proven
comprehensive
Free Assessment
86% of our members feel better within 12 weeks.
We accept insurance.





FREQUENTLY ASKED QUESTIONS
If your question isn’t answered below, view our full list of FAQs here.
Brightside is available to people 18 years and older in the states where Brightside operates who believe they may be experiencing depression and may benefit from treatment.
Remote care is not a good fit for people with certain conditions or situations. These include (but are not limited to):
Our providers do not treat, and do not prescribe for adhd.
If any of these describe you, it’s best for you to be seen by a provider in person so you can get the care that’s right for you.
Brightside makes it easy to get top quality depression care from the privacy of home.
Here’s how Psychiatry works:
Here’s how Therapy works:
When scheduling your first appointment, you can browse all of our available providers in your state. Take a look at their profiles and check open times to find the best fit for you. Every Brightside provider undergoes a rigorous hiring and vetting process to ensure the highest quality care.
Brightside currently accepts select insurance plans in various states for payment of your provider’s or therapist’s services. Please see below for a current listing of plans. Brightside may not be included in all plans that each health insurance company offers. Please contact your health insurance plan to verify that your care at Brightside will be covered.
We currently accept the following insurance plans:
If you are a new member signing up for services you can enter your insurance information during the sign-up process. We’ll let you know your eligibility, as well as you estimated co-pays and out-of-pocket costs (if any) before signing-up or scheduling.
We also accept HSA/FSA payment if you have one of those accounts. If you have questions about using your medical or prescription insurance benefits, please contact us by emailing [email protected].
The onset of a specific phobia is complex, and there are a few different causes and risk factors at play. These include:
However, it is important to remember that learning is not the sole cause of specific phobias. Many people are bitten by dogs or get into car accidents and do not go on to develop phobias.
Risk factors for phobias may also include a genetic component, but not much is known about the biological factors that cause and maintain specific phobias. What we do know is that when someone encounters a feared stimulus, many biological changes occur in the body, including changes in brain activity, the release of cortisol, insulin, and growth hormone, and increases in blood pressure and heart rate.
If you have a specific fear or phobia that is interfering with your everyday life, it might be time to make an appointment to see your doctor. If left untreated, phobias can interfere with your personal relationships and prevent you from functioning normally at home, school, or work.
A medical provider will diagnose you with a phobia based on the following criteria:
The medical provider is likely to ask about current symptoms and family history, particularly whether other family members have had phobias. You may want to report any experience or trauma that may have triggered the phobia (i.e., a dog bite leading to a fear of dogs).
It may be helpful to discuss how you react—your thoughts, feelings and physical symptoms— when you are confronted with the thing you fear. It might also be helpful to describe what you do to avoid fearful situations, and how the phobia affects your daily life, including your job and your personal relationships.
Phobias are typically treated using a combination of medication and therapy.
Medication
Short-term medication is sometimes prescribed to treat the side effects of phobias, such as anxiety or panic attacks. If the phobia is confronted only occasionally, as in a fear of flying, the use of medication can be limited.
Antidepressants are often prescribed to help reduce the anxiety associated with phobias. Selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs) are most often prescribed to treat anxiety, social phobia, or panic disorder.
Therapy
Cognitive behavioral therapy (CBT) can help ease the symptoms of a phobia—especially when a technique called exposure therapy is implemented. Exposure therapy involves gradually increasing your exposure to the thing you fear, at your own pace, under controlled circumstances. As you are exposed to the object, you are taught to master your fear through various strategies including relaxation, breathing control, or other anxiety-reducing techniques.
Self-Care, Coping, and Support
Many treatment plans for phobias involve aspects of self-care. This can include: